… and a Fortnight
 After nearly three months, a lot of my stay in the hospital is a blur and I don’t remember the names of most of the staff anymore. But what I do remember was that all the nurses and CNA’s (Certified Nursing Assistants) were very caring and supportive. All of them were good and most were excellent. Not once did I detect any measure of negativity towards me because I was transgender.
After nearly three months, a lot of my stay in the hospital is a blur and I don’t remember the names of most of the staff anymore. But what I do remember was that all the nurses and CNA’s (Certified Nursing Assistants) were very caring and supportive. All of them were good and most were excellent. Not once did I detect any measure of negativity towards me because I was transgender.
One major change for me since I transitioned is that I have a much more positive attitude towards medical situations and personnel than I used to have. Yes, if I am truly in pain, I will not hide that fact. But I try to be pleasant, even cheery and I can even tell a joke or two, sometimes in the midst of pain. Hopefully the hospital staff came away with a good feeling after interacting with me with each shift.
Every so often, I had a few moments to chat with one of the staff members. With one we talked about dealing with psoriasis. Another time, I shared about probably having played high school baseball against Denzel Washington. With another, I shared about my talent to imitate popular singers (although not enough breath to do it at the time and not sure if I will still be able to do so when I get dentures). I remember explaining to one nurse the meaning of “cisgender” and talking about transgender issues in general. Another staff member told me about some differences in Dr. McGinn’s protocol. And shortly before I was about to be released, I had an emotional moment with an understanding CNA who had another staff member wait while I had “a moment”: talking about what my surgery meant to me, how fortunate I had been to not have any negative public incidents in the five years since I had begun presenting as Lois to the world and how bad I felt for my transgender sisters who haven’t been so fortunate.
That’s not to say that everything went perfectly. The machines which monitored the drip from my IV bags beeped far more often than they should have. One staff member told me that they never worked properly. But I never wanted to ignore that beeping for long. So I rang the nurse’s station more often than I would have liked, probably 90% of the time for that reason.
 My operation was on a Thursday. Business must have been slow because on Friday evening around 5 PM, I got a ride to a different wing of the hospital on that floor. So few beds were occupied that they shut down the wing I was on and consolidated the patients. That wasn’t a problem. The problem was when the nurse went into my closet and didn’t find my belongings there. They never came up with me from where they had been put before surgery. And because it was now the weekend, it was much harder to find someone to bring my bag to me. I had some jellied candies in it that I would have loved to eat at times when I had an appetite and no food in sight. And I had some pocket testaments that I would have loved to have offered to some of the staff. (If the conversation went in certain directions, I was not shy letting staff know that I am a Christian.) I was only reunited with my belongings about 15 minutes before I was discharged on Sunday.
My operation was on a Thursday. Business must have been slow because on Friday evening around 5 PM, I got a ride to a different wing of the hospital on that floor. So few beds were occupied that they shut down the wing I was on and consolidated the patients. That wasn’t a problem. The problem was when the nurse went into my closet and didn’t find my belongings there. They never came up with me from where they had been put before surgery. And because it was now the weekend, it was much harder to find someone to bring my bag to me. I had some jellied candies in it that I would have loved to eat at times when I had an appetite and no food in sight. And I had some pocket testaments that I would have loved to have offered to some of the staff. (If the conversation went in certain directions, I was not shy letting staff know that I am a Christian.) I was only reunited with my belongings about 15 minutes before I was discharged on Sunday.
Then there was the food: do not go to the hospital for the food. To be honest, I didn’t have much of an appetite for a couple of weeks after the operation. Furthermore, I don’t understand the Romans wanting to be fed while lying on a couch. Breakfast in bed doesn’t seem to be much of a luxury for me anymore. In summation, the food was edible (and sometimes better than that) and occasionally I was hungry.
 There was also a matter of timing. We were served at 8 AM, Noon and 5 PM. There was also a shift change at 8 AM. One night, I ended up horizontal instead of slanted at my usual 30º angle. I rang for someone to put me into position to eat breakfast. It didn’t happen until 9 AM. And I enjoyed that breakfast (French toast with bacon, as I recall, and both were very good). But lunch three hours later was too soon. And there was always a long gap between dinner and next morning’s breakfast.
There was also a matter of timing. We were served at 8 AM, Noon and 5 PM. There was also a shift change at 8 AM. One night, I ended up horizontal instead of slanted at my usual 30º angle. I rang for someone to put me into position to eat breakfast. It didn’t happen until 9 AM. And I enjoyed that breakfast (French toast with bacon, as I recall, and both were very good). But lunch three hours later was too soon. And there was always a long gap between dinner and next morning’s breakfast.
Somehow by around 10:30 on Sunday morning, October 8, I was reunited with all my belongings, I had calmed down from my “moment” and one of my dearest trans women friends came to take me from the hospital to the recovery room at Dr. Leis’s office. Since she had two of her children with her, I don’t know if she wants me to identify her by name. But since she reads my blog, she can certainly do so if she wants to and if it won’t cause a problem for her. And she knows that when it is time for her recovery from surgery, I will be there for her.
Slowly getting to my feet for the first time since Thursday morning, I managed to navigate the distance from my bed to the wheelchair and the walk from wheelchair to front seat of her car, while being cognizant of having to carefully handle the catheter bag. While it was nice to get out of bed and out of the hospital in general (even as wonderful as everyone was), if I had my druthers I’d rather have stayed in place until that catheter had been taken out.
And so I made the return trip from Bristol to Bala Cynwyd during daylight hours on a gray, drizzly, cool morning. The GPS took us a different way than Dr. Leis used, a combination of I-95, US 13 and US 1. There were lots of places with bumpy pavement (and the occasional railroad track) and after major surgery I was much more aware of those bumps than I was on Thursday morning.
Then we got to the doctor’s office and confusion. I thought someone on staff was meeting me. And I thought that Dr. Leis would examine me at some point, maybe even when I arrived. (I didn’t see him at any point while in the hospital after the operation.)
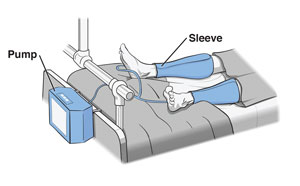
But when we arrived, no one was there. I finally reached the doctor on his cell phone and he told us to just go straight to the recovery room. He saw me that evening. So I gingerly made my way up the stairs with my thighs feeling like they had turned to lead in three days. During the hospital portion of recovery, Dr. Leis uses SCD’s (sequential compression device) on the calves in lieu of walking early to prevent blood clots (plus an injection of blood thinner), but they do nothing to stimulate the thighs. Having been told that everyone manages to do it, I pressed on and made it.
The most important thing I can tell you if you are facing GRS or any other major internal surgery in the future is that every person’s body reacts differently. They can only tell you what happens in most cases. Your mileage may vary.
Dr. Leis had told me that it would be a few days before I would have a bowel movement. Jenna told me that for a while I would have a feeling of pressure like I was having a bowel movement, but it wasn’t one for the first few days. The hospital staff doctor who checked me and pronounced that I was fit to be discharged told me that I wouldn’t have a bowel movement for a few days.
Even so, I had experienced a watery discharge from my bowels the day after the operation. It had come on my quite suddenly, too fast for the nurses to get there when I rang for them. So I got to experience what it is like to have your hospital bedding changed when you are in the bed. I’m sure it isn’t their favorite job, but they are quite proficient at it. And fortunately for them, I’m more featherweight than heavyweight.
Now I am in the recovery room in Bala Cynwyd. I wasn’t able to get anyone to stay with me for the first day (my friend who chauffeured me had to leave for a family event) and there is no one staying in the adjoining room. Jenna is going to come at some point and make something for me to eat but she hasn’t arrived yet. I have finally figured out which remote will change the channels and I am looking forward to watching some playoff baseball.
You know how you are warned on the passenger side mirror that things aren’t what they seem to be? Well I had been told that something that felt like a bowel movement wasn’t really a bowel movement. But by golly it sure felt like one. And finally I decided I couldn’t take the chance. It was a good thing I moved when I did. Dragging a catheter and moving at a reduced pace and trying to avoid soiling the floor, I made it over the toilet bowl just in time. (Of course, I was in the room furthest from the bathroom, but it was the room out of the two where the TV worked.) I couldn’t get the outer dressing out of the way in time, but I did the best I could. Sorry Jenna! At least I was wise enough not to flush and clog the plumbing with the dressing. With rubber gloves, the packing could be retrieved (and was). I think I finally convinced Jenna that I didn’t put the dressing in the toilet on purpose. Hopefully by now she realizes it could have been much worse. And life went on.
I got good news early on. I was told that my friend Carolyn (wife of college classmate, Blair) had rearranged her schedule to come a day earlier than originally planned. Actually she did more than rearrange. She cancelled some piano lessons (paying customers) on Monday so she could come a day earlier. Blair stopped in when they arrived and it was great to see them both.
All of my caregivers were wonderful. But of the three, Carolyn was the only one who had children. So she was the most experienced caregiver at a time when I needed the most care. And she figured out how to empty the Foley catheter bag, a strange contraption of clamps, tubes and storage compartments that seems to be illogically configured at first, second and third glance. (I had done it when no one else was there, but very clumsily and it was difficult for me to explain it.)
Dr. Leis showed me how to change the dressings when the catheter was in, and more importantly, once the catheter was removed. The removal caused an interesting sensation and a moment of pain when it popped out, but then it was over. I have been told to be glad that I never needed a penile catheter.
Carolyn was there from Monday to Saturday. In between sleep, watching television, reading, phone calls, meal prep and Carolyn’s daily walk, we had many interesting conversations. GRS in itself is somewhat surreal, even as much as it was important for me. But it was also surreal to be having deep conversations with her. My mind flashed back to having similar deep conversations with Blair, sometimes to the wee hours of the morning, whether about life in general or what we were going through in terms of relationships, school or career. Those conversations were ostensibly guy to guy. Now I am having woman to woman conversations with his wife. I am blessed to have two such wonderful friends and conversationalists in my life.
 Carolyn was my caregiver (although she excused herself) when the catheter came out. That was when I was handed the mirror and got a glimpse of the Dr. Leis’s handiwork for the first time. The raw tissue and stitches were still very visible, but at least from the outside, I now look female there. That wasn’t surreal. It was very matter of fact. I started to change my dressings with two non-woven sponges (that look more like gauze pads to me), covered with what is known as either a combine pad or an ABD pad. And I learned how to pull up what Dr. Leis calls “granny panties” (aka wings) over them to serve as my disposable underwear.
Carolyn was my caregiver (although she excused herself) when the catheter came out. That was when I was handed the mirror and got a glimpse of the Dr. Leis’s handiwork for the first time. The raw tissue and stitches were still very visible, but at least from the outside, I now look female there. That wasn’t surreal. It was very matter of fact. I started to change my dressings with two non-woven sponges (that look more like gauze pads to me), covered with what is known as either a combine pad or an ABD pad. And I learned how to pull up what Dr. Leis calls “granny panties” (aka wings) over them to serve as my disposable underwear.
Most of all, I had a surge of delight when Dr. Leis (clinically, of course), described my genitalia as “your urethra”, “your clitoris”, “your vagina”, “your vulva” and “your labia”. This was my actual skin and tissue, not some prosthetic device.
While Carolyn was there, I got a visit from an aesthetician that Dr. Leis provides for his trans women patients recovering from GRS (perhaps others as well). She told me that she could come back on Friday. It would be a time of pampering, I was told. She would arrive between 1:30 and 2:30 in the afternoon. My friend Deirdre also called me to tell me she would be coming to visit on Friday afternoon. Gauging the traffic and when she could leave, she expected to arrive around 4 and 4:30 PM. No conflict, right?
Of course, the aesthetician arrived at 2:30 or even a few minutes after. And Deirdre, even after a stop at Murray’s Deli, was early. The traffic between DC and Philly must have set a record for lightest ever on a Friday afternoon. And my tablet is ringing with her phone call while I am covered with a skin treatment and can’t get to it.
As far as the aesthetician, all I will say is that sometimes two people just do not hit it off. I get along with almost everyone. After all I move comfortably in very conservative Christian circles and very liberal LGBT circles. But she and I, after the first few minutes, just did not click. What was supposed to be a pleasant, relaxing pampering experience turned out to be the opposite. In fact, I was somewhat agitated and talked to Deirdre and Carolyn about it a few times after the aesthetician left. Plus the session cut short my visiting time with Deirdre, which in retrospect I would have much preferred. (Fortunately Deirdre and Carolyn, both having music backgrounds, had friends in common and had a lovely conversation in the next room.)
Margaret, my friend from sixth grade, followed Carolyn in the caregiver role from Saturday to Monday. Despite my telling them not to bring food (I had enough there to feed Sherman’s army and with me off my feed, it lasted longer than expected), they both did. But it was good and we enjoyed it.
My friend Jamee (a former engineering co-worker of Blair and a client of mine until she retired) took the final caregiving shift. Jamee met me for the first time a couple of years before I transitioned and she and I just hit it off immediately. It was also great to get to know her better as one can do when sharing a room for three days. We also had some great conversations.
Jamee also helped make a key decision for me. Dr. Leis wanted to see me before sending me home. But he was delayed on Wednesday. By the time he arrived and checked me out, it was past time for us to have dinner. While Jamee had started to load the car for me (she was a blessing in that department), we hadn’t finished. She told me that she could stay until the following morning and suggested I stay rather than leave and get home late. It was an excellent suggestion. So that’s what we did.
Mid-morning on Thursday October 19, I headed for home. Wanting to avoid stopping to go to the bathroom if possible so I wouldn’t have to do a dressing change in a public bathroom (I eventually became quite good at doing so), I made excellent time and found myself home in a little over two hours. But by then, I really did need to use the facilities. I took care of business and then rushed back downstairs because I had cold food in the car that needed to be refrigerated. From the exertion, I barely got inside my apartment when I passed out. Fortunately, I grabbed hold of a quilt nearby and slid rather than fell.
I revived, put the food away and went to sleep rather than try to bring the rest of my things upstairs. In fact, that would take a while and was done gradually over the next week or two. The next day, October 20, I would have my next irreversible surgery of the month: all my teeth were being pulled in preparation for dentures. As of this writing, due to complications in my healing, I expect to be without usable teeth and on a soft food diet for about three months before I have wearable dentures. But that is an entirely different story.
I will have one more blog post in this series, dealing with the aftermath of the operation, evaluations and recommendations.
Remember ye not the former things, neither consider the things of old. Behold, I will do a new thing; now it shall spring forth; shall ye not know it? I will even make a way in the wilderness, and rivers in the desert. – Isaiah 43:18-19
God bless,
Lois